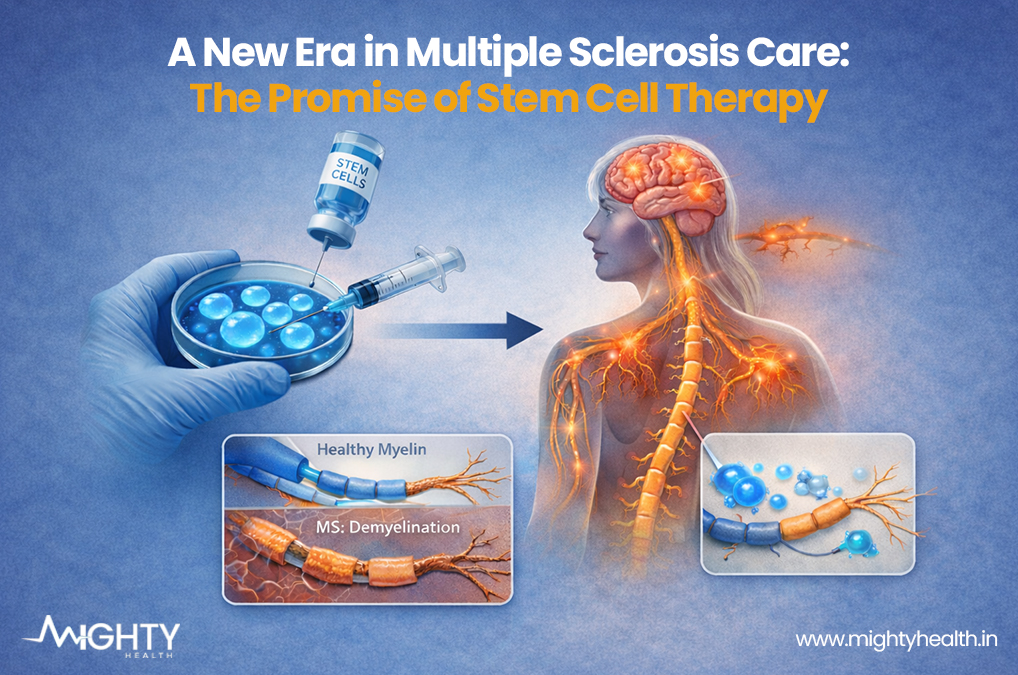
Understanding Multiple Sclerosis
Multiple sclerosis is caused by an immune system attack against the myelin sheath. This myelin sheath surrounds nerve fibres in both the brain and spinal cord, and when myelin gets damaged, messages sent from the brain to the body get disrupted. In addition to disruptions in the communication between the brain and body, disruption of the myelin sheath can lead to an MS sufferer having fatigue, numbness, problems with vision, mobility problems, issues with memory or thinking.
Most doctors currently use disease-modifying therapies (DMTs) to treat multiple sclerosis. DMTs work by suppressing the immune response to the disease and/or reducing inflammation in the body. Many patients respond positively to DMTs, but they do not provide a cure for MS, and often do not provide results to patients with the progressive form of MS. As a result, researchers are looking at alternative treatment options such as regenerative therapies and immunotherapy (stem cells).
What Is Stem Cell Therapy?
Due to their ability to reproduce themselves and also to become several kinds of organised bodily tissues, stem cells are very special cells. Stem cells being able to do this makes them a prime choice for spoiling and regulating abnormal immune systems.
When speaking about multiple sclerosis (MS) and stem cells, usually, when stem cells and multiple sclerosis are discussed, the term (stem cell therapy) is applied to the following:
Autologous Hematopoietic Stem Cell Transplantation (AHSCT)
Here’s how it works: Doctors collect a patient’s own blood-forming stem cells, freeze them, and then give the patient powerful immunosuppressive treatment. After that, they put the stem cells back.
The idea is pretty simple—wipe out the immune cells that are attacking myelin, and then let the body build a fresh set of immune cells that don’t go after the nervous system.
Research backs this up. AHSCT stops disease activity and helps a lot of people with relapsing MS stay in remission, especially if they’re younger and still dealing with inflammation.
Mesenchymal Stem Cell (MSC) Therapy
MSCs come from places like bone marrow, fat tissue, or umbilical cords. Doctors can give them through an IV or put them straight into the cerebrospinal fluid.
The idea here is to calm inflammation, release protective substances, and maybe even help nerves heal.
Some clinical trials show people get better neurological function and fewer active lesions after getting MSCs, but the results aren’t as consistent as what we see with AHSCT.
Emerging & Experimental Approaches
Neurogenesis (neural stem cells) and the use of stem cell-derived extracellular vesicles are other strategies that may help directly repair damaged neural circuits. Clinical studies are still limited at this time to demonstrate their efficacy to date.
How Stem Cell Therapy Works
Before getting into why stem cell therapy shows so much promise for MS, it makes sense to look at what’s actually going on behind the scenes.
Immune Resetting
AHSCT is basically a hard reset for your immune system. Doctors wipe out the troublemaker cells that attack your own body, then bring in stem cells to rebuild a new, hopefully calmer immune system. The goal here is simple: stop those immune attacks that trigger MS flare-ups.
Neuro-Modulation and Neuroprotection
MSCs have this interesting ability—they release growth factors and other signals that cool down inflammation and nudge the brain to start repairing itself. This doesn’t just dial back the damage; it also helps protect neurons that are still hanging in there, giving your brain a better shot at recovery.
Myelin Regeneration (What’s Next)
Here’s where things get exciting, at least in the lab. Animal studies show that some types of stem cells, like induced neural stem cells, can actually move into damaged spots in the brain or spinal cord and start making new myelin. That’s huge—because instead of just slowing MS down, we’re talking about reversing some of the damage. It’s early days, but this shift in thinking could change everything about how we treat MS down the road.
What the Evidence Says: Clinical Progress & Outcomes
Stem cell MS therapies have been transitioned into practical use with real clinical trials, particularly in AHSCT, at least in part due to increasing research:
AHSCT: Effectiveness Evidence.
AHSCT is emerging as an alternative with regard to the most promising option for patients with a highly active relapsing-remitting MS (RRMS) who are not responding to the conventional therapies.
Follow-up studies in the long term show that a large percentage of the patients still do not progress the disease many years after treatment.
MSC Therapy: Safety and Preliminary Results.
The safety profile of MSC therapy is favourable, and initial clinical trials indicate that MSC therapy causes a decrease in inflammatory markers and slight improvements in disability scales.
Nonetheless, more extensive and more rigorous studies are required to demonstrate a similar degree of effectiveness, particularly between various types of MS.
Limitations and Gaps
There are numerous studies that continue to rely on limited sample sizes and limited follow-up.
There has not been a universal consensus on standardised procedures (e.g. cell type, dosage, delivery method).
The research indicates that there is greater strength in the cessation of disease activity compared to the restoration of lost neurological activity.
Who Could Benefit Most?
Stem cell therapy isn’t right for everyone with MS, but here’s who seems to benefit most:
- People who have highly active relapsing MS, especially RRMS.
- Those who just aren’t getting better with strong standard treatments.
- Younger folks who haven’t had MS for long and have less disability.
- Some people with secondary progressive MS, but usually only in clinical trials.
The bottom line? Stem cell treatment isn’t something you just jump into. You need a full medical workup, and only specialists in neurology and transplants should be guiding the process.
Risks and Considerations: What Patients Should Know
There is no want of risks in the stem cell treatments:
Treatment-Related Risks
AHSCT is associated with immunosuppressive chemotherapy that is highly fatiguing and is linked to such risks as infection, adverse complications related to treatment, and, in extreme cases, severe adverse events.
MSC therapies are considered to be safer, yet they also need close medical attention.
Variable Outcomes
Not every patient is a good respondent. Others can enter remission or improvement phase, whereas others can benefit to some extent. The long-term effects are still under investigation.
Need for Specialised Care
In case of stem cell therapies, it must be done in certified medical facilities that have experience in MS and transplantation procedures. The best and most convenient method of accessing state-of-the-art treatment is through participation in clinical trials.
The Future of MS Care: What’s On the Horizon?
Stem cell therapy isn’t just exciting because of what it can do now—it’s the possibilities down the road that really get people talking.
New Ways to Heal
Scientists are digging into neural stem cells and things like extracellular vesicles. The hope? Real myelin repair and actual nerve healing, not just tweaking the immune system.
Tailored Treatments
With advances like AI-powered biomarkers and better ways to sort out different types of MS, doctors are getting closer to matching the right stem cell therapy to the right person.
Mixing It Up
Looking ahead, treatment probably won’t be one-size-fits-all. Picture stem cells working alongside targeted drugs, neuroprotective therapies, and rehab—all teaming up for better results.
Let’s Wrap Up
The advent of stem cell therapy opens new doors for some patients with multiple sclerosis (MS). It has the potential to reset the immune system, decrease inflammation, and possibly promote regeneration of nerve cells - things that current treatments cannot do. This gives patients hope. However, both physicians and researchers are erring on the side of caution by waiting for more definitive results, longer follow-up studies, and guidelines before using stem cells routinely.
For those who live with MS and care for someone with MS there is an exciting yet realistic expectation for what is to come through stem cell therapy; there is no "magic bullet" in this case - stem cell therapy represents a developing pathway toward a different type of MS treatment that focuses on providing healing, personalized treatment programs, and tangibly improving a person's ability to function day to day.